Maternal Health
For every woman who dies, an estimated 20 or 30 encounter injuries, infections, or disabilities. Most of these deaths and injuries are entirely preventable.
Making motherhood safer is a human right imperative at the core of Doctors On Call’s mandate.
Doctors On Call work worldwide with other non-governmental organizations, health experts, and civil society to train health workers, improve the availability of essential medicines and reproductive health services, strengthen health systems, and promote international maternal health standards.
Making motherhood safer is a human right imperative at the core of Doctors On Call’s mandate.
Doctors On Call work worldwide with other non-governmental organizations, health experts, and civil society to train health workers, improve the availability of essential medicines and reproductive health services, strengthen health systems, and promote international maternal health standards.
Significant strides, but not enough
Doctors On Call work worldwide with other non-governmental organizations, health experts, and civil society to train health workers, improve the availability of essential medicines and reproductive health services, strengthen health systems, and promote international maternal health standards.
Most maternal deaths are preventable. In 2017, an estimated 295,000 women died of causes related to pregnancy or childbirth. Most died from severe bleeding, sepsis, eclampsia, obstructed labor, and the consequences of unsafe abortions – all reasons for which highly effective interventions exist. And the tragedy does not stop there: When mothers die, their families are much more vulnerable, and their infants are more likely to die before their second birthday.
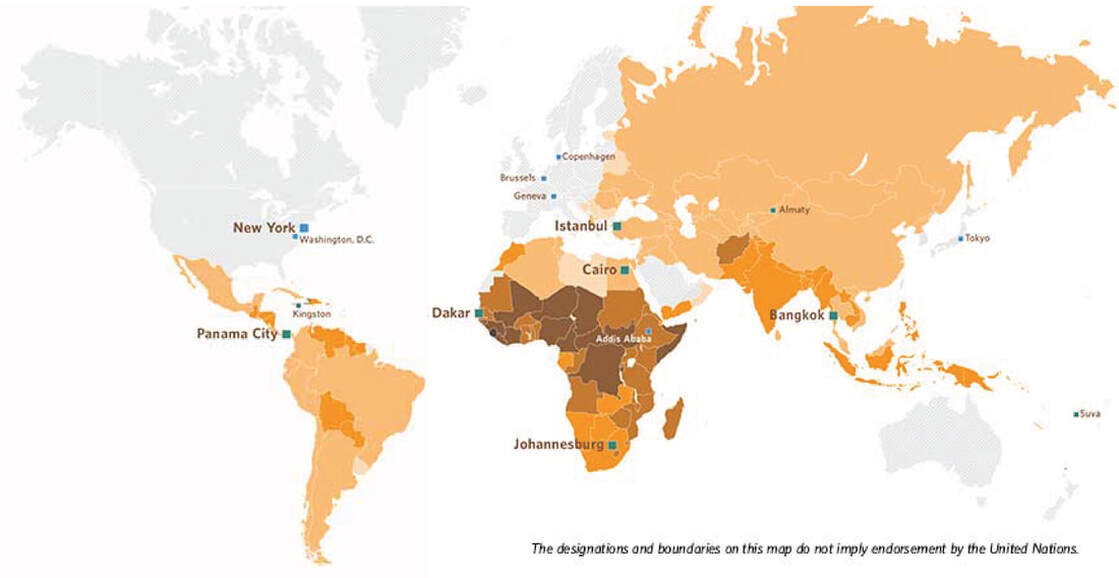
But much more must be done. High rates of maternal mortality persist, particularly in impoverished communities. Of the hundreds of thousands of women who died during pregnancy or childbirth in 2017, approximately 86 percent lived in sub-Saharan Africa and Southern Asia.
Most maternal deaths are preventable. In 2017, an estimated 295,000 women died of causes related to pregnancy or childbirth. Most died from severe bleeding, sepsis, eclampsia, obstructed labor, and the consequences of unsafe abortions – all reasons for which highly effective interventions exist. And the tragedy does not stop there: When mothers die, their families are much more vulnerable, and their infants are more likely to die before their second birthday.
But much more must be done. High rates of maternal mortality persist, particularly in impoverished communities. Of the hundreds of thousands of women who died during pregnancy or childbirth in 2017, approximately 86 percent lived in sub-Saharan Africa and Southern Asia.
Complications of pregnancy or childbirth
For every woman who dies from pregnancy-related causes, 20 to 30 experience chronic or acute morbidities. A potentially fatal condition complicates up to 15 percent of all births. Women who survive such complications often require lengthy recovery and may face lasting physical, psychological, social, and economic consequences. Although many of these complications are unpredictable, almost all are treatable.
These conditions can kill, disable, or lead to stillbirths without treatment. The costs of medical care and lost productivity can also drive women and their families into poverty. Obstetric fistula, for example, can result in chronic infections, social isolation, and deepening poverty.
These conditions can kill, disable, or lead to stillbirths without treatment. The costs of medical care and lost productivity can also drive women and their families into poverty. Obstetric fistula, for example, can result in chronic infections, social isolation, and deepening poverty.
Antenatal care
Prenatal care is an integral part of primary maternal health care. It is recommended that expectant mothers receive at least four antenatal visits, in which a health worker can check for signs of ill health – such as underweight, anemia, or infection – and monitor the fetus's health. During these visits, women are counseled on nutrition and hygiene to improve their health before and after delivery. They can also develop a birth plan, an essential component of antenatal care, which lays out how to reach care and what to do in an emergency.
Because these visits may be a woman’s first interaction with the health system, they are an important opportunity to assess her overall health and to speak with her about her sexual and reproductive health and rights. In these settings, women learn the health benefits of spacing births and how to plan their families. They are also counseled on newborn care and the importance of birth registration.
Still, most complications arise with little or no warning among women with no risk factors. While antenatal visits may not prevent complications, women who receive antenatal care are more likely to deliver with the help of a skilled birth attendant who can recognize and address these issues.
Because these visits may be a woman’s first interaction with the health system, they are an important opportunity to assess her overall health and to speak with her about her sexual and reproductive health and rights. In these settings, women learn the health benefits of spacing births and how to plan their families. They are also counseled on newborn care and the importance of birth registration.
Still, most complications arise with little or no warning among women with no risk factors. While antenatal visits may not prevent complications, women who receive antenatal care are more likely to deliver with the help of a skilled birth attendant who can recognize and address these issues.
Skilled birth attendance
With emergency backup, skilled attendance at birth is considered the most critical intervention for ensuring safe motherhood. Skilled birth attendants are health workers, such as doctors, nurses, or midwives, who have the skills to manage regular deliveries and recognize the onset of complications. They perform essential interventions, start treatment, manage primary complications, and supervise other complications to comprehensive emergency care. Skilled attendance is also vital for protecting newborns’ health, as most perinatal deaths occur during delivery or 48 hours afterward.
Skilled attendance requires an enabling environment, such as a clean delivery area with the necessary supplies and equipment. And skilled birth attendants must provide respectful care that considers the pregnant woman's dignity. Unfortunately, many countries have severe shortages of trained health providers with midwifery skills.
Skilled attendance requires an enabling environment, such as a clean delivery area with the necessary supplies and equipment. And skilled birth attendants must provide respectful care that considers the pregnant woman's dignity. Unfortunately, many countries have severe shortages of trained health providers with midwifery skills.
Emergency obstetric care
Emergency obstetric care is critical to reducing maternal mortality. All five major direct causes of maternal death – hemorrhage, sepsis, unsafe abortion, hypertensive disorders, and obstructed labor – can be treated at a well-staffed, well-equipped health facility. Many newborns with asphyxia or infection can also be saved in such settings.
In case of complications, all women and newborns should have rapid access to well-functioning emergency obstetric facilities meeting good quality-of-care standards. And in the long term, all births should occur in appropriate facilities, as is the case in countries with significantly reduced maternal mortality.
In case of complications, all women and newborns should have rapid access to well-functioning emergency obstetric facilities meeting good quality-of-care standards. And in the long term, all births should occur in appropriate facilities, as is the case in countries with significantly reduced maternal mortality.
Post-natal care
Post-natal care – provided within the first 24 hours of delivery, on the third day afterward, then in the second and sixth weeks – is as important as antenatal care. Bleeding, sepsis, and hypertensive disorders can all occur after a woman has exited the health center. And newborns are also extremely vulnerable in the immediate aftermath of birth.
UNFPA strongly recommends follow-up visits by a health worker to assess the mother and child’s health post-natal period.
UNFPA strongly recommends follow-up visits by a health worker to assess the mother and child’s health post-natal period.
FOCUS
Our involvement is to make motherhood a safe journey. DOC promotes universal access to sexual and reproductive health care and rights by promoting international maternal health standards and providing guidance and support to health systems.
DOC helps train midwives, supports emergency obstetric and newborn care facilities and networks, and provides essential drugs and services.
Doctors On Call focuses on making pregnancy and childbirth as safe as possible in emergencies.
DOC helps train midwives, supports emergency obstetric and newborn care facilities and networks, and provides essential drugs and services.
Doctors On Call focuses on making pregnancy and childbirth as safe as possible in emergencies.
Subscribe for NEWSLETTER |